Overview
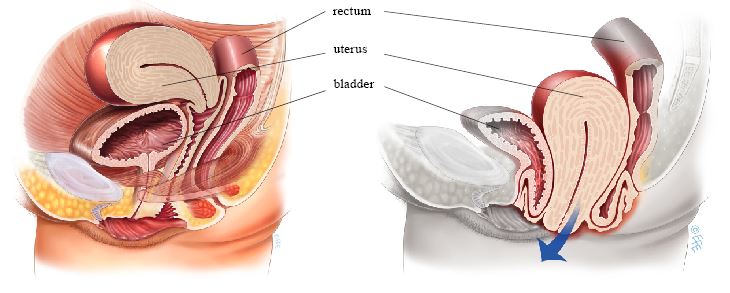
Vaginal hysterectomy is removal of the uterus through the vagina without any abdominal incisions. It is the preferred approach for hysterectomy when feasible, and is often performed as part of prolapse repair surgery. It may be combined with anterior repair, posterior repair, and apical suspension procedures.
Indications
- Uterine prolapse requiring surgical treatment
- Abnormal uterine bleeding
- Symptomatic fibroids (when vaginal approach is feasible)
- Completed childbearing with symptomatic pelvic organ prolapse
Advantages
- No abdominal incisions or scars
- Faster recovery compared to abdominal hysterectomy
- Shorter hospital stay
- Lower postoperative pain
The Procedure
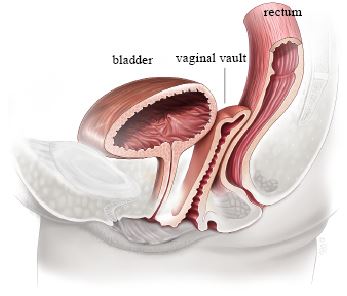
The uterus is detached from its supporting structures and removed through the vagina. The ovaries may be preserved or removed depending on individual factors. A vaginal vault suspension procedure is performed to support the top of the vagina and prevent future vault prolapse.
Recovery
- Hospital stay: typically 1-2 nights
- Return to light activities: 1-2 weeks
- Full recovery: approximately 6 weeks
- Sexual intercourse: usually after 8 weeks
- Light vaginal bleeding or spotting may occur for several days
Post-Operative Expectations
Following hysterectomy, menstrual periods will stop. If both ovaries are removed before natural menopause, surgical menopause will occur. Decisions regarding ovarian conservation are individualized.
Risks and Success Rates
Vaginal hysterectomy achieves an 85% permanent cure rate for uterine prolapse. There is approximately a 15% risk of developing vaginal vault prolapse months or years later. Potential risks include:
- Occult urinary incontinence — correction of the prolapse may unmask underlying stress incontinence in 40-45% of patients
- Urinary retention — 10-15% of patients in the early post-operative period
- Urinary tract infection — 6-20% of patients
- Vaginal vault hematoma — approximately 10%
- Bleeding requiring transfusion — 0-10% depending on the complexity of the procedure
- Injury to bladder, ureters, or rectum — up to 2%
- Vaginal or pelvic infection — uncommon
- Venous thromboembolism — rare
Illustrations courtesy of the International Urogynecological Association (IUGA) Patient Information Leaflets.