Overview
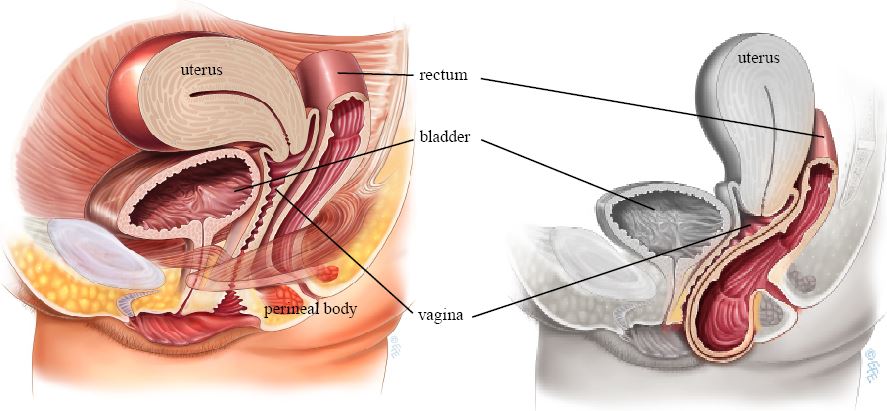
Posterior colporrhaphy (posterior repair) is a vaginal surgical procedure to correct prolapse of the back wall of the vagina (rectocele), where the rectum bulges into the vaginal canal. It may be combined with perineorrhaphy (repair of the perineal body) when there has been perineal descent.
Indications
- Symptomatic posterior compartment prolapse (rectocele)
- Difficulty with bowel movements, incomplete emptying, or needing to splint (press on the vaginal wall) to evacuate
- Vaginal bulge causing discomfort
The Procedure
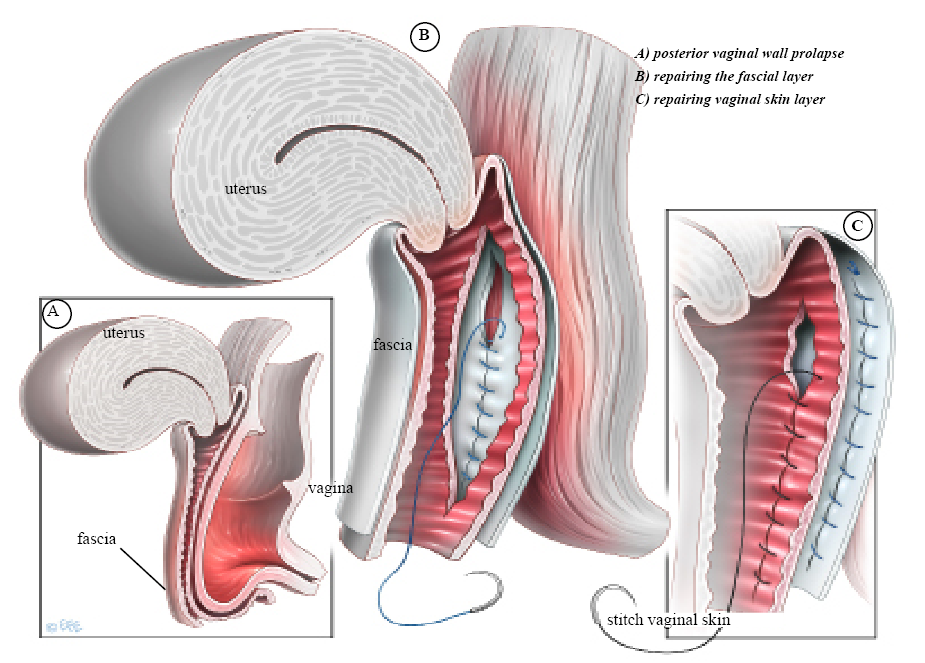
An incision is made in the back wall of the vagina. The tissue between the vagina and rectum (rectovaginal fascia) is identified and reinforced with stitches. If a perineorrhaphy is also performed, the perineal muscles are reapproximated. Excess vaginal tissue may be trimmed, and the incision is closed.
Recovery
- Hospital stay: typically 1 night
- Return to light activities: 1-2 weeks
- Full recovery: approximately 6 weeks
- Bowel function may take a few days to normalize — stool softeners are usually recommended
- Sexual intercourse: usually after 8 weeks
Risks and Success Rates
Posterior vaginal wall repair has an 80-90% success rate. Approximately 50% of women with pre-existing incomplete bowel emptying or constipation experience improvement after surgery. Potential risks include:
- Prolapse recurrence — the prolapse may return over time
- Urinary tract infection — approximately 6% of patients
- Dyspareunia — some women may develop discomfort during intercourse
- Constipation — common in the short-term after surgery
- Bleeding requiring transfusion — less than 1%
- Rectal injury — very uncommon but possible during surgery
Posterior repair is commonly performed in combination with other prolapse procedures.
Illustrations courtesy of the International Urogynecological Association (IUGA) Patient Information Leaflets.