Overview
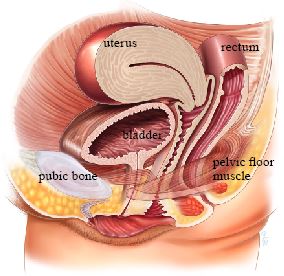
A pessary is a removable silicone device inserted into the vagina to provide mechanical support for pelvic organ prolapse or to reduce stress urinary incontinence. Pessaries are a safe, effective, and reversible treatment option that can be used as temporary or long-term management.
Indications
Pessaries are most suitable if you:
- Wish to delay or avoid surgery
- Have not completed childbearing
- Have medical conditions that increase surgical risk
- Prefer a non-surgical approach
- Want to maintain daily function while awaiting surgery
Types of Pessaries

Pessaries come in various shapes and sizes:
- Ring pessary — the most commonly used type, suitable for mild to moderate prolapse. Some versions include a support shelf.
- Gellhorn pessary — provides stronger support for more advanced prolapse
- Cube pessary — used for more severe prolapse
- Incontinence pessary — specifically designed to support the urethra and reduce stress incontinence
Fitting
Pessaries require fitting by your healthcare provider and may require some trial and error before the most suitable size and type is found. It is possible to remain sexually active with some types (such as ring pessaries).
Ongoing Care
- Pessaries require periodic follow-up, typically every 3-6 months
- Some patients learn to remove, clean, and reinsert their pessary independently
- Vaginal estrogen may be recommended alongside pessary use to maintain vaginal tissue health
- Possible side effects include vaginal discharge, odor, or irritation, which are generally manageable
Risks and Considerations
Vaginal pessaries are a safe and effective non-surgical option for managing prolapse. Potential issues include:
- Vaginal discharge — most women experience a small amount of whitish discharge, which may increase with certain pessary types
- Vaginal irritation or ulceration — can occur depending on pessary type and fit, causing pinkish or bloody discharge
- Discomfort — usually indicates incorrect sizing and can be resolved with refitting
- Regular follow-up — pessaries require periodic removal, cleaning, and assessment of the vaginal tissues
Illustrations courtesy of the International Urogynecological Association (IUGA) Patient Information Leaflets.