Overview
Pelvic floor muscle training (PFMT) aims to improve strength, coordination, and endurance of the pelvic floor muscles. These exercises are the cornerstone of conservative management for urinary incontinence, fecal incontinence, and pelvic organ prolapse. Treatment is often guided by trained pelvic floor physiotherapists who provide individualized programs with regular assessment.
How It Works
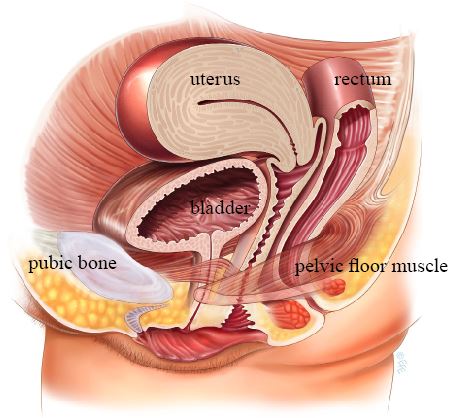
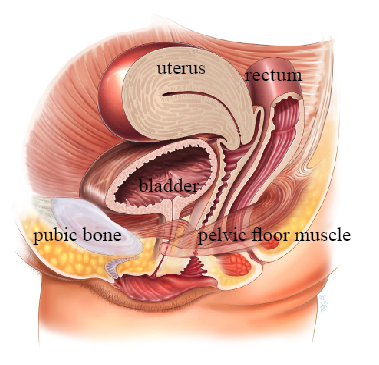
The pelvic floor comprises a group of muscles that form a supportive platform between the tailbone and pubic bone. These muscles support the bladder, uterus, and rectum, and help control the release of urine and stool. When these muscles weaken — due to childbirth, aging, menopause, or other factors — symptoms such as urinary leakage, pelvic heaviness, and bowel control difficulties may develop.
PFMT involves learning to identify, contract, and relax these muscles correctly. Proper technique is essential, as many women initially perform the exercises incorrectly without professional guidance.
Conditions Treated
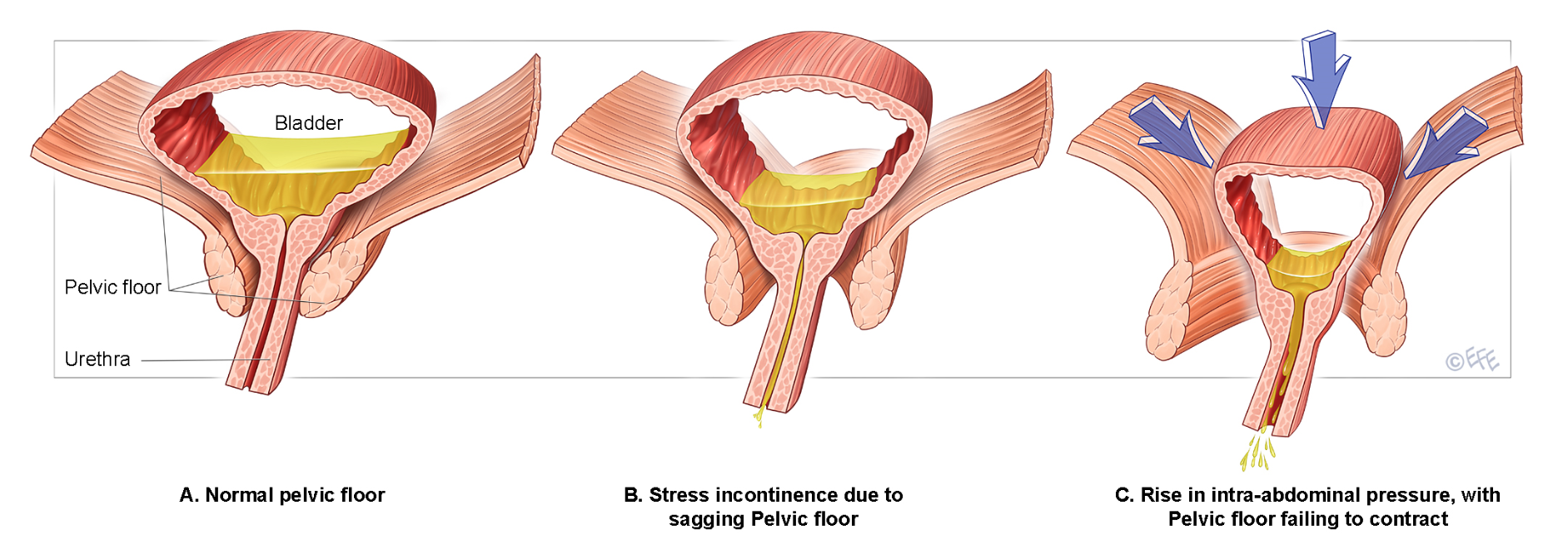
- Stress urinary incontinence
- Urgency urinary incontinence and overactive bladder
- Mixed urinary incontinence
- Mild to moderate pelvic organ prolapse
- Fecal incontinence
- Chronic pelvic pain (relaxation and down-training)
- Pre- and post-surgical optimization
What to Expect
A pelvic floor physiotherapist will:
- Assess your pelvic floor muscle strength, coordination, and endurance
- Develop a personalized exercise program
- Teach correct technique (biofeedback may be used)
- Monitor progress and adjust the program over time
Maximum benefit typically occurs after 3 to 6 months of regular exercise. Up to 75% of women with stress incontinence show improvement with supervised PFMT.
At-Home Practice
Between appointments, you will practice exercises at home. Consistency is key — like any exercise program, the benefits depend on regular practice over time. Your physiotherapist will provide guidance on the number and frequency of exercises.
Important Considerations
- PFMT is recommended as first-line treatment before considering surgical options
- For women with pelvic pain, the focus may be on relaxation rather than strengthening
- Pre-surgery pelvic floor training can improve outcomes after prolapse or incontinence surgery
Effectiveness
Supervised pelvic floor muscle training can produce major improvement in or recovery from stress urinary incontinence symptoms in many women, potentially avoiding or delaying the need for surgery. Improvement may begin at 3–6 weeks, but it can take up to 6 months to achieve full benefit. Correct technique is essential — performing exercises incorrectly may be counterproductive. There are no significant risks associated with pelvic floor physiotherapy when performed correctly.
Illustrations courtesy of the International Urogynecological Association (IUGA) Patient Information Leaflets.