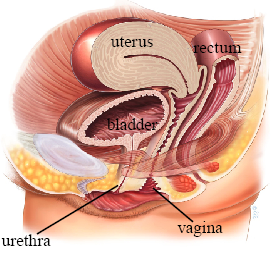
Overview
A midurethral sling is a synthetic mesh tape placed under the middle section of the urethra to provide support during activities that increase abdominal pressure (coughing, sneezing, exercise). It is the most commonly performed surgical procedure for stress urinary incontinence, with 80-90% cure or significant improvement rates.
Approaches
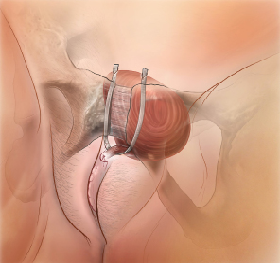
Retropubic Sling (Gold Standard)
The tape passes under the urethra through the retropubic space, exiting through two small skin incisions just above the pubic bone. This is the most studied approach with extensive long-term data.
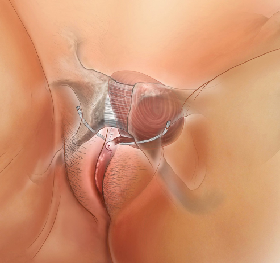
Transobturator Sling
The tape runs under the urethra and passes through the obturator foramen, exiting through small incisions in the groin creases. Effective with a slightly different risk profile (less risk of bladder injury, slightly higher risk of groin discomfort).
Both approaches are effective, with small differences in risk profiles. The choice is based on clinical factors and surgeon recommendation.
The Procedure
- Performed under general or regional anesthesia
- Small incision in the vaginal wall beneath the urethra
- Sling positioned tension-free beneath the mid-urethra
- Typically a day-surgery procedure
- Procedure time: approximately 20-30 minutes
Recovery
- Most women recover within 2-4 weeks
- Some groin discomfort (especially with transobturator) may last a couple of weeks
- Light vaginal bleeding for 7-10 days is not unusual
- Return to full activity including exercise: approximately 4-6 weeks
Important Information
This procedure is designed to treat stress incontinence. It does not cure urgency incontinence or overactive bladder, although up to 50% of women notice some improvement in urgency symptoms. In a small percentage of women with OAB, symptoms may worsen.
Risks include a small chance of mesh exposure, voiding difficulty (temporary or requiring further intervention), and discomfort.
Risks and Success Rates
Midurethral sling procedures have an 80-90% patient satisfaction rate, with most women reporting that their incontinence is cured or significantly improved. Long-term data for the retropubic approach (TVT) shows sustained effectiveness for at least 17 years when the initial procedure is successful. About 50% of women with pre-existing urgency symptoms also experience improvement. Potential risks include:
- Mesh exposure — occurs in 2-4% of cases and may present weeks, months, or years after surgery
- Voiding difficulty — 1-5% of women experience temporary difficulty passing urine, usually resolving within the first week
- Bladder perforation — occurs in 1-5% of retropubic (TVT) procedures; the rate is lower with the transobturator approach
- New or worsened urgency — approximately 5% of patients develop new urgency or urge incontinence
- Post-operative pain — approximately 1% with retropubic sling; up to 10% with transobturator sling (typically groin pain)
- Urethral perforation — 1% or less, more associated with the transobturator approach
- Urinary tract infection — common in the early post-operative period