Overview
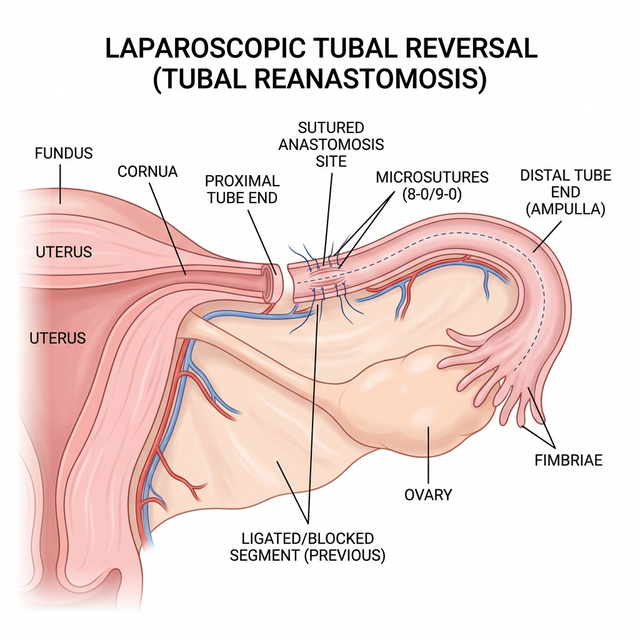
Laparoscopic tubal reversal (tubal reanastomosis) is a microsurgical procedure to reconnect the fallopian tubes after a previous tubal ligation (sterilization). The goal is to restore the natural pathway for the egg and sperm to meet, allowing the possibility of natural conception without the need for in vitro fertilization (IVF).
Indications
- Desire to conceive naturally after previous tubal ligation
- Suitable tubal anatomy with adequate remaining tubal length (generally ≥ 4 cm after reconnection)
- An alternative to IVF for appropriately selected patients
Pre-operative Assessment
Before proceeding with tubal reversal, a thorough assessment is performed to determine suitability:
- Review of operative records: To determine the method and site of the original tubal ligation
- Ovarian reserve testing: Blood tests (AMH, FSH) to assess remaining egg supply
- Semen analysis: Evaluation of the partner's fertility
- Pelvic ultrasound: To assess uterine and ovarian anatomy
- Age and fertility counselling: Success rates are significantly influenced by age, with best outcomes in women under 35
Surgical Technique
- Performed under general anesthesia using a laparoscopic approach with microsurgical instruments
- 3–4 small abdominal incisions (5–12 mm)
- The blocked or ligated segments of the fallopian tube are identified, trimmed, and the healthy tubal ends are precisely realigned
- The tubal lumen is reconnected in two layers using fine microsurgical sutures (6-0 to 8-0) under magnification
- Tubal patency is confirmed intraoperatively by chromopertubation (dye test through the cervix)
- Operative time is typically 90–150 minutes
What to Expect After Surgery
- Usually performed as a day surgery procedure; some patients stay overnight
- Mild pelvic discomfort for several days, managed with simple analgesia
- Return to light activities within 1–2 weeks
- Full recovery: approximately 2–4 weeks
- Attempts at natural conception may begin after 2–3 months, once healing is confirmed
- A hysterosalpingogram (HSG) may be performed at 3 months to confirm tubal patency
Success Rates
Pregnancy rates after laparoscopic tubal reversal depend on several factors:
- Age: Women under 35 have the highest success rates (60–80% pregnancy rate within 1–2 years)
- Type of original ligation: Clip or ring sterilization generally has better outcomes than procedures that destroy longer segments of tube
- Remaining tubal length: Longer remaining segments are associated with higher success
- Time since ligation: Does not significantly impact outcomes if tubal anatomy is favorable
Tubal Reversal vs. IVF
The choice between tubal reversal and IVF depends on individual circumstances. Tubal reversal may be preferred when:
- Multiple pregnancies are desired (each cycle provides an opportunity to conceive naturally)
- Age and tubal anatomy are favorable
- The patient prefers natural conception
IVF may be preferred when:
- Tubal anatomy is unfavorable for successful reconnection
- There are additional fertility factors (male factor, diminished ovarian reserve)
- The patient is over 38 years of age
Risks and Success Rates
The success of tubal reversal depends on several factors including the method of original sterilization, the length of remaining fallopian tube, and the patient's age. Pregnancy rates after reversal vary from approximately 40–80% depending on these factors. Potential risks include:
- Ectopic pregnancy — the risk is higher after tubal reversal than in the general population; any positive pregnancy test should be evaluated early
- Failure to achieve pregnancy — reversal does not guarantee fertility
- Bleeding — occasionally requiring transfusion
- Injury to surrounding structures — uncommon
- Infection — wound or pelvic infection
- Adhesion formation — scar tissue may affect tubal function