Overview
Sacrocolpopexy is a surgical procedure that suspends the vaginal apex (or the uterus/cervix in uterine-preserving approaches) to the sacrum (a bone at the base of the spine) using synthetic mesh. When performed laparoscopically, it offers the benefits of the abdominal approach with a faster recovery.
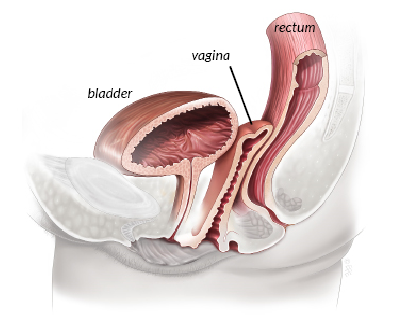
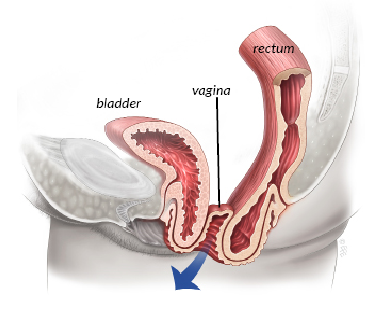
Why Sacrocolpopexy?
Sacrocolpopexy is considered the gold standard for apical prolapse repair because it offers:
- Best long-term anatomical durability for apical prolapse
- Lower recurrence rates compared to vaginal native tissue repairs
- High patient satisfaction in appropriately selected cases
- 90-95% long-term success rates
Indications
- Symptomatic apical (vault or uterine) prolapse
- Recurrent prolapse after prior vaginal repair
- Women who wish to maintain sexual function
- Patients suitable for general anesthesia and a laparoscopic approach
The Procedure
- Performed through small abdominal incisions under general anesthesia
- A lightweight polypropylene mesh is attached to the front and/or back wall of the vagina
- The mesh is then secured to the sacral promontory (a bony landmark on the sacrum)
- The peritoneum is closed over the mesh to reduce contact with the bowel
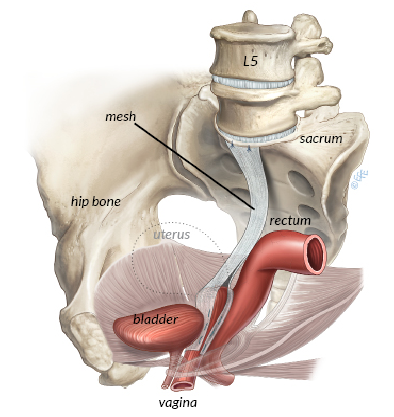
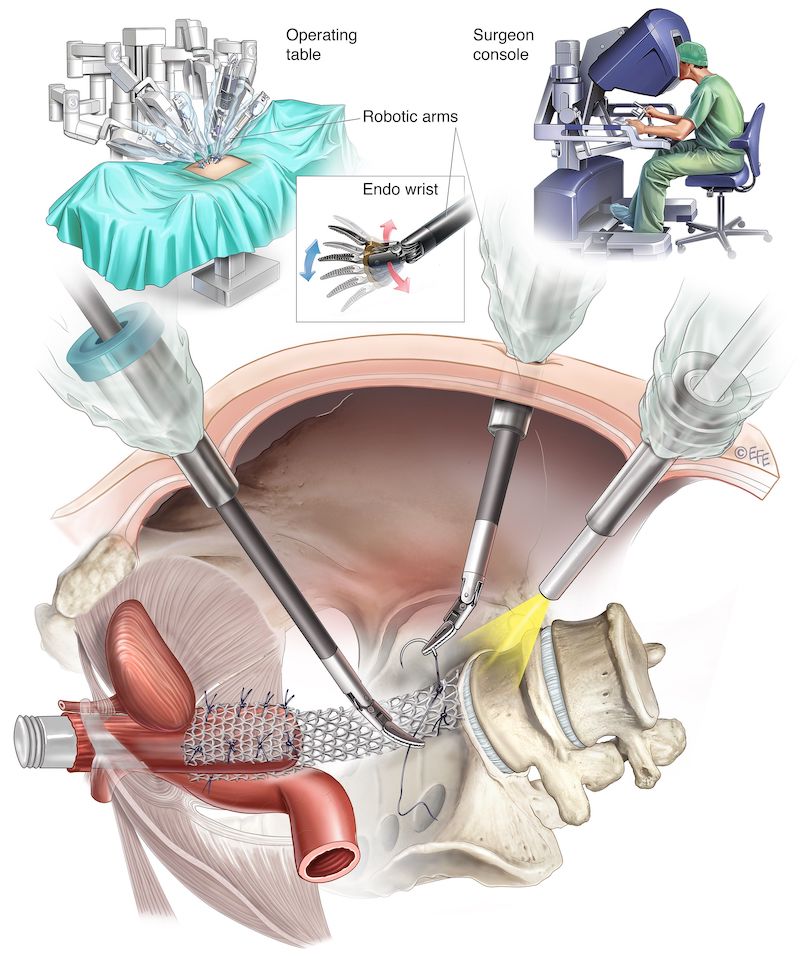
May be combined with other procedures such as anterior or posterior repair, anti-incontinence surgery, or hysterectomy if indicated.
Recovery
- Hospital stay: typically 1-2 nights
- Return to light activities: 2-3 weeks
- Full recovery: approximately 6 weeks
- Sexual intercourse: usually after 8 weeks
Considerations
- Use of permanent mesh: there is a small risk (approximately 2-4%) of mesh exposure or erosion, usually at the vagina
- Longer surgery compared to vaginal approaches
- Small risk of injury to surrounding structures
- Not suitable for all patients — the choice between sacrocolpopexy and vaginal repair is individualized
Risks and Success Rates
Laparoscopic sacrocolpopexy has an 80-90% success rate for curing prolapse and associated symptoms. It is considered the gold standard for apical prolapse repair due to its long-term durability. Potential risks include:
- Mesh exposure or erosion — occurs in approximately 2-4% of cases, most commonly at the vaginal apex, and may require a further procedure
- Voiding difficulty — up to 10% of patients may experience temporary difficulty emptying the bladder in the early post-operative period, usually resolving within weeks
- Pain or discomfort during intercourse — reported in 2-5% of patients
- Constipation or bowel dysfunction — occurs in approximately 2-3% of cases
- Injury to bladder, bowel, or ureters — occurs in 1-2% of cases
- General surgical risks — including urinary tract infection, wound infection, bleeding requiring transfusion, and venous thromboembolism
Illustrations courtesy of the International Urogynecological Association (IUGA) Patient Information Leaflets.