Overview
Apical suspension procedures support the top of the vagina (vaginal vault) or the uterus/cervix by anchoring them to strong ligaments or bony structures within the pelvis. These are essential components of prolapse surgery, as adequate apical support is the foundation of a durable repair.
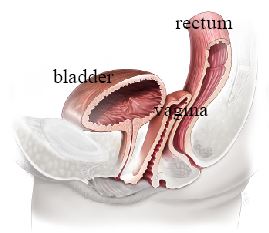
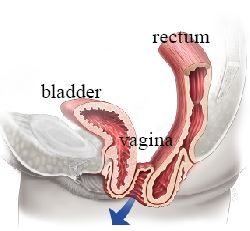
Uterosacral Ligament Suspension
The vaginal apex or cervix is sutured to the uterosacral ligaments — strong native ligaments that naturally support the uterus. This can be performed vaginally or laparoscopically.
Advantages:
- Uses native tissue (no mesh)
- Re-establishes the natural axis of the vagina
- Can be combined with other vaginal repairs
Considerations:
- Small risk (approximately 1-3%) of ureteral kinking requiring intraoperative correction
- Cystoscopy is routinely performed during the procedure to confirm ureteral function
Sacrospinous Ligament Fixation
The vaginal apex is sutured to the sacrospinous ligament, a strong ligament deep in the pelvis. This is performed through a vaginal approach.
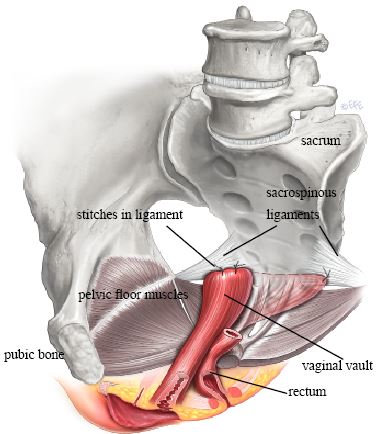
Advantages:
- No abdominal incisions
- Well-established procedure with good long-term results
- Particularly useful in combination with vaginal hysterectomy
Considerations:
- May result in a slightly posterior deviation of the vaginal axis
- Temporary buttock or leg pain may occur due to proximity to nerves (usually resolves within weeks)
Recovery
- Hospital stay: typically 1-2 nights
- Return to light activities: 1-2 weeks
- Full recovery: approximately 6 weeks
Risks and Success Rates
Apical suspension procedures achieve an 80-90% success rate for correcting vault or uterine prolapse. The specific risk profile depends on the technique used.
Sacrospinous fixation:
- Buttock pain — approximately 10% of women in the early post-operative period, usually self-limiting
- New stress urinary incontinence — develops in approximately one-third of patients
- Voiding difficulty — approximately 10% experience ongoing difficulty with bladder emptying
Uterosacral ligament suspension:
- Ureteric injury — 1-10% of cases; intraoperative cystoscopy may be performed to check
- Urinary tract infection — 7-34% depending on catheter use
- Buttock pain — usually short-term
Common risks for both procedures:
- Prolapse recurrence or development in another compartment
- Dyspareunia — rare; most women report improved sexual function
- Bleeding requiring transfusion — uncommon
- Venous thromboembolism — rare
Illustrations courtesy of the International Urogynecological Association (IUGA) Patient Information Leaflets.