What is Stress Urinary Incontinence?
Stress Urinary Incontinence (SUI) is the involuntary leakage of urine during activities that increase abdominal pressure, such as coughing, sneezing, laughing, lifting, or exercising. SUI affects at least 10-20% of women, many of whom do not realize that there are simple, effective treatment options available.
SUI affects women's quality of life in many ways. Incontinence may limit social and personal relationships as well as physical activity.
How Does the Normal Bladder Work?
As urine fills the bladder, the bladder (detrusor) muscle relaxes and stretches to accommodate the fluid. When the bladder is filled to a certain level, an urge to pass urine is felt. The brain then signals the detrusor muscle to contract and the urethral sphincter to relax, allowing urine to be passed. The bladder usually needs to be emptied about 5-7 times per day and 1-2 times at night.
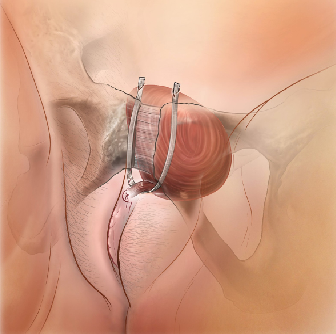
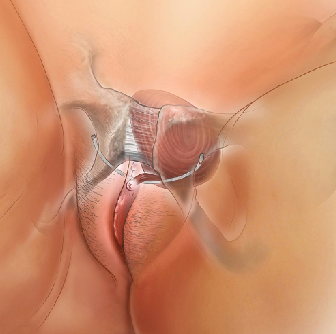
The urethra and bladder are supported by the pelvic floor muscles, which contract during coughing, sneezing, and exercise to prevent leakage. Weakness in the muscles or damage to bladder neck support can result in leakage.
Causes
- Pregnancy and vaginal birth — direct injury to the pelvic floor support structures
- Obesity, chronic cough, heavy lifting, and constipation — increased abdominal pressure that aggravates stress incontinence
- Genetic factors — inherited predisposition to weaker connective tissues
- Menopause — hormonal changes that affect tissue integrity
Diagnosis
Your physician will ask questions about activities that cause leakage and will examine you to assess for any related problems, such as prolapse. Diagnostic steps may include:
- Cough stress test: Your doctor may ask you to cough with a comfortably full bladder to observe leakage.
- Bladder diary: A record of how much you drink, how often you void, the volume passed each time, and how much leakage occurs.
- Urodynamic studies: Investigate the bladder's ability to fill and empty, and the mechanism of the incontinence.
- Ultrasound scan: To determine how much urine remains in the bladder after emptying and to identify other causes of symptoms.
- Urinalysis: To rule out urinary tract infection.
Non-Surgical Treatment
Conservative treatment is usually recommended as the initial approach:
- General lifestyle changes: Drink enough to pass urine 4-6 times per day (usually about 1.5-2 liters). Maintaining weight within a healthy range has been shown to reduce the severity of SUI. Avoiding constipation and quitting smoking can also help.
- Pelvic floor exercises: Pelvic floor muscle training (Kegel exercises) can be very effective, with up to 75% of women showing improvement. Maximum benefit usually occurs after 3 to 6 months of regular exercise. A pelvic floor physiotherapist can supervise your training.
- Continence devices: Vaginal devices that help control leakage, inserted prior to exercise or worn continuously.
Surgical Treatment Options
When conservative treatments have been tried and are insufficient, surgical options may be considered:
Midurethral Sling
A synthetic mesh sling is placed under the urethra to provide support during increases in abdominal pressure. This is the most commonly performed procedure, with 80-90% success rates.
- Retropubic approach — the gold standard
- Transobturator approach — effective with a slightly different risk profile
Burch Colposuspension
A laparoscopic procedure using sutures for urethral support. Effective but takes longer and may be slightly less effective than mesh sling procedures.
Autologous Fascial Sling
Uses the patient's own tissue (fascia) from the abdomen or thigh. Highly effective (80-90%) but carries a higher risk of postoperative voiding difficulty.
Urethral Bulking Injections
Material is injected around the urethra to improve closure. Best suited for mild stress incontinence or patients who are not surgical candidates. Lower success rates and often requires repeat treatments.
When to Seek Help
If urinary leakage is affecting your daily activities or quality of life, many effective treatment options are available. Dr. Kruger can provide a thorough evaluation and create a personalized treatment plan.