What is Overactive Bladder?
Overactive bladder (OAB) is a very common condition that causes distressing and inconvenient symptoms. It can cause you to rush to the toilet many times during the day and night, and sometimes causes urine leakage before reaching the toilet.
OAB is the name given to the following collection of bladder symptoms:
- Urgency — a sudden and intense need to pass urine that cannot be put off, even when your bladder is not full. If you do not make it to the toilet in time and leak, this is called urge incontinence.
- Frequency — going to the toilet many times during the day (usually more than 7 times).
- Nocturia — waking up more than once at night to go to the toilet.
OAB affects women and men of all ages and is not simply a result of getting older.
How Does it Happen?
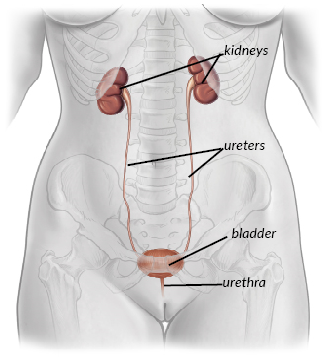
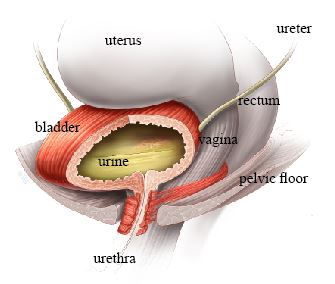
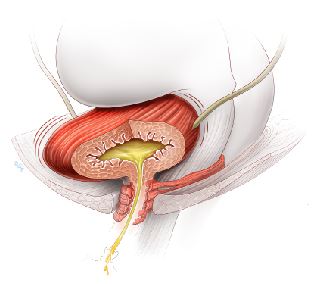
OAB symptoms are caused by the bladder muscle squeezing to empty out urine inappropriately. This often happens without warning and when you do not want it to.
Causes
Your doctor will test your urine to rule out an infection, which is a common cause of OAB symptoms. Other contributing factors include:
- Conditions affecting the nervous system
- Previous surgery for stress incontinence
- The amount and type of liquids you drink (caffeinated drinks significantly worsen OAB symptoms)
- Bladder stones or growths
For many women, the exact cause of their OAB is never found. Despite this, there are many treatments which can help manage symptoms.
Diagnosis
When you see your doctor, they will ask about your bladder function, fluid intake, and general health. You will be examined to rule out any contributing gynecological problems. Diagnostic tests may include:
- Urinalysis — to check for infection or blood in the urine
- Residual urine measurement — using ultrasound to check whether you are emptying your bladder properly
- Urodynamic studies — to examine bladder muscle activity as it fills, determine if detrusor overactivity is present, and assess bladder emptying
Treatment Options
Lifestyle Modifications
Caffeinated drinks (coffee, tea, cola) can significantly worsen OAB. Fizzy drinks, fruit juices, and alcohol can also contribute. Try keeping a bladder diary to identify which drinks make symptoms worse. Switch to water, herbal teas, and decaffeinated drinks. Aim to drink about 1.5-2 liters per day — do not cut down on total fluid intake.
Bladder Training
Gradually increasing the time between visits to the toilet helps your bladder hold more urine. It involves trying to hold on for a little longer if you experience the urge to empty, gradually extending the interval. Your doctor or physiotherapist can guide you through this treatment.
Pelvic Floor Exercises
Pelvic floor muscle training improves the ability to suppress urgency and helps reduce leakage episodes.
Medications
Several medications can help with an overactive bladder. They enable you to hold on longer, reduce frequency, and decrease leaking. Side effects such as dry mouth or constipation may occur. Sometimes you may need to try several different drugs before finding one that suits you. Your bladder may improve after a few months of treatment, allowing you to come off the medication, though many women need longer-term therapy.
Advanced Treatments
For symptoms that persist despite conservative measures:
- Botulinum toxin injections: Injected into the bladder via cystoscopy under local anesthetic, causing relaxation of the bladder muscle. Up to 80% effective, lasting approximately 9 months before repeat treatment may be needed. There is a 10-20% risk of temporary difficulty emptying the bladder.
- Tibial nerve stimulation: Stimulates the nerves that control bladder function via a nerve near the ankle, retraining bladder behavior.
- Sacral neuromodulation: A nerve stimulator is implanted to directly stimulate the nerves controlling bladder function. Offered for severe, persistent symptoms that have not responded to other treatments.