What is Mixed Urinary Incontinence?
Mixed urinary incontinence refers to the presence of both stress and urgency urinary incontinence. Women with this condition experience urine leakage both during physical activities (coughing, sneezing, exercise) and with sudden, intense urges to urinate. Mixed incontinence is very common and affects a significant proportion of women seeking treatment for urinary symptoms.
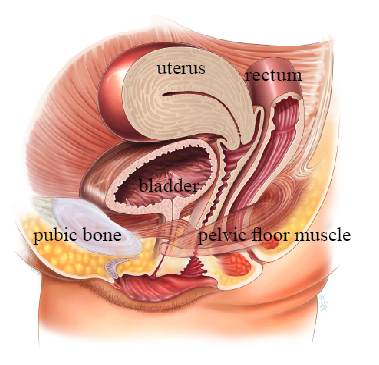
Understanding the Two Components
Stress Component
Leakage occurs with physical movements that increase abdominal pressure. This is related to weakness of the pelvic floor muscles and urethral support structures, often resulting from childbirth, aging, or connective tissue changes.
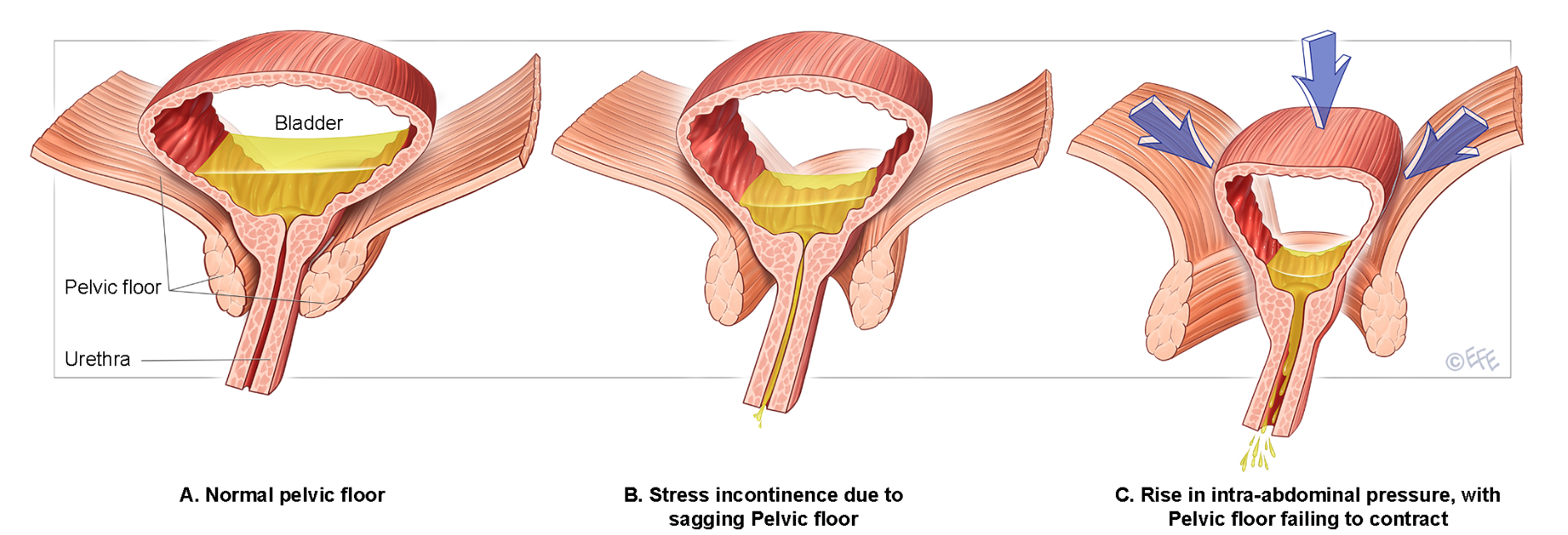
Urgency Component
Leakage is associated with a sudden, compelling need to void that is difficult to defer. This is caused by involuntary bladder muscle contractions (detrusor overactivity) that may be triggered by various factors.
Evaluation
Assessment begins with a detailed clinical history to understand the relative contribution of each component. Understanding which type of leakage is most bothersome helps guide treatment priorities.
Evaluation may include:
- Detailed symptom questionnaire to characterize the pattern and severity of each component
- Bladder diary recording fluid intake, voiding frequency, and leakage episodes
- Physical examination including pelvic floor assessment
- Urodynamic studies to confirm the underlying mechanisms of incontinence, particularly when surgical treatment is being considered
Management
Treatment generally involves addressing both components through a stepwise approach:
Conservative Management (First-Line)
- Pelvic floor muscle training — improves both stress and urgency symptoms
- Bladder training — helps retrain the bladder to hold more urine and suppress urgency
- Lifestyle modification — weight management, fluid optimization, reduction of bladder irritants (caffeine, alcohol), and management of constipation
- Vaginal estrogen therapy — may improve tissue health and reduce both stress and urgency symptoms in postmenopausal women
Pharmacotherapy
- Anticholinergic or beta-3 agonist medications may be added to address the urgency component, often in conjunction with ongoing pelvic floor exercises
Surgical Intervention
When conservative measures are insufficient, treatment of the dominant symptom is usually addressed first. If stress incontinence is the predominant concern, surgical options such as a midurethral sling may be considered. The urgency component may improve, persist, or occasionally worsen after surgery for stress incontinence.
What to Expect
Management is individualized based on which component is most bothersome, symptom severity, and patient preferences. Many women achieve significant improvement with conservative treatment alone.
Illustrations courtesy of the International Urogynecological Association (IUGA) Patient Information Leaflets.