What is GSM?
The Genitourinary Syndrome of Menopause (GSM) is a collection of symptoms that impact the genital and urinary tracts in women as a consequence of hormonal changes during menopause. These symptoms can have a significant effect on quality of life and intimate relationships. GSM likely affects more than half of menopausal women.
Unlike hot flashes, another common menopause symptom, GSM does not improve over time in postmenopausal women. Similar symptoms can also occur in premenopausal women and others with low estrogen, including those in the postpartum period.
Symptoms
- Vaginal dryness and irritation
- Pain during sexual intercourse (dyspareunia)
- Urinary frequency, urgency, and burning with urination
- Recurrent urinary tract infections
- Changes in vaginal discharge
Causes
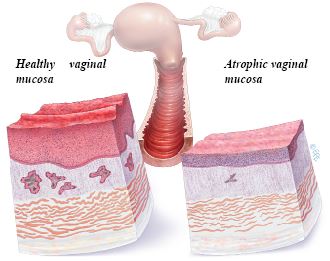
GSM is primarily driven by the decline in estrogen levels during menopause. Estrogen is important for maintaining the health and elasticity of vaginal and urinary tissues. As estrogen decreases, these tissues become thinner, drier, and more prone to irritation. The decline in estrogen also affects the vaginal environment, including the normal bacterial flora and pH. Because the urethra and bladder also have estrogen receptors, low estrogen levels cause urinary symptoms and increase UTI risk.
Diagnosis
Diagnosing GSM involves a comprehensive assessment by your healthcare provider. Other conditions (overactive bladder, urinary tract infections, vaginal infections) can cause similar symptoms and may coexist with GSM.
- Medical history review to understand your symptoms
- Physical examination including a pelvic exam
- Laboratory and additional tests as needed to rule out other conditions
Treatment Options
Non-Hormonal Treatments
- Vaginal moisturizers: Applied regularly to address dryness. Some contain hyaluronic acid for extended moisture retention.
- Lubricants: Used prior to intercourse. Available in water-based, oil-based, and silicone-based formulations.
- Regular sexual activity: Helps maintain vaginal elasticity.
- Vaginal dilators and vibrators: Help maintain tissue elasticity and reduce discomfort.
Hormonal Treatments
- Local vaginal estrogen: Low-dose estrogen applied directly to the vaginal tissues is a safe and effective method to alleviate dryness and discomfort. Available as creams, tablets, or rings. Local estrogen is generally considered safe even for women with a history of breast cancer after discussion with their care team.
- DHEA: Has been shown to be effective for GSM when applied locally.
- Systemic estrogen therapy: Can help with both systemic menopausal symptoms and GSM, though for GSM symptoms alone, local estrogen is preferred.
- Selective Estrogen Receptor Modulators (SERMs): Such as ospemifene, an oral medication that can restore hormonal balance to the vagina.
Improvement with hormonal treatments may take a few weeks to months to become apparent. Treatment is typically continued long-term as symptoms will recur when treatment is stopped.
Illustrations courtesy of the International Urogynecological Association (IUGA) Patient Information Leaflets.