What is Interstitial Cystitis / Bladder Pain Syndrome?
Interstitial cystitis (IC), also known as Bladder Pain Syndrome (BPS), is a chronic condition characterized by bladder pain or discomfort with a frequent and urgent need to pass urine. Nine in ten people with IC are women. The condition is not caused by bacterial or viral infection and is considered a diagnosis of exclusion.
People with IC may have a bladder wall that is inflamed and irritated. In severe cases, the bladder wall inflammation can scar and stiffen the bladder so it cannot easily expand as it fills. Some women develop pinpoint bleeding of the bladder wall when stretched or have ulcers of the bladder lining which may lead to pain, urinary frequency, and urgency.
Symptoms
- An urgent need to urinate, both when awake and asleep, which may be difficult to defer
- A frequent need to urinate out of proportion to liquid consumption
- Pressure, pain, and tenderness around the bladder, pelvis, and perineum that often increases as the bladder fills and decreases as the bladder empties
- A bladder that does not hold as much urine as it did before
- Pain during sexual intercourse
Symptoms vary greatly between individuals and even in the same person over time. Many women find that symptoms worsen before their menstrual period. Stress may also make symptoms worse, but it does not cause the condition.
What Causes IC/BPS?
While we do not currently know the exact causes, possible contributing factors include:
- Defective bladder lining: In about 70% of people with IC, the protective inner lining of the bladder is "leaky," allowing urine to irritate the bladder wall
- Increased histamine release: An inflammatory process that results in IC symptoms
- Increased nerve cells: Heightened sensitivity of the bladder wall
- Autoimmune process: Antibodies acting against part of the body
Diagnosis
IC is a diagnosis of exclusion. Your doctor will assess your symptoms, perform testing, and rule out other conditions including urinary tract infections, bladder stones, vaginal infections, and bladder cancer.
Diagnostic steps may include:
- Detailed symptom assessment
- Urinalysis
- Cystoscopy: A special telescoping camera to look inside the bladder and identify inflammation, pinpoint bleeding, or ulcers
- Bladder diary
- Urodynamic testing in selected cases
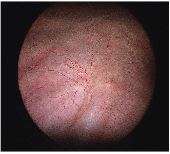
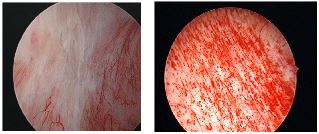
Treatment Options
Because the causes are not fully understood, current treatments are aimed at relieving symptoms. One or a combination of treatments helps most people:
Dietary Modifications
Avoid alcohol, spicy and acidic foods, chocolate, caffeine, citrus drinks, artificial sweeteners, and tomatoes. Try eliminating these foods for several weeks, then reintroduce one at a time to identify triggers.
Bladder Training
If bothered by frequency or urgency without significant pain, bladder training with gradually increasing intervals between voiding may help.
Physical Therapy
People with IC often have painful spasms of the pelvic floor muscles. A physiotherapist can teach exercises to both strengthen and relax the pelvic floor, and techniques such as biofeedback may be helpful.
Medications
- Pentosan polysulfate — Helps protect the bladder wall lining. About 40% of patients improve (an ophthalmology exam is recommended before starting due to a rare associated eye condition).
- Amitriptyline — Blocks pain and reduces bladder spasms. Usually taken at bedtime as it may cause drowsiness.
- Antihistamines — May help when inflammation has an allergy-based component.
Bladder Instillations
A catheter is used to fill the bladder with liquid medicine (such as heparin, steroids, local anesthetic, or DMSO) held for up to 15 minutes. Treatments are typically given weekly for 6-8 weeks and can be repeated.
Bladder Distension
A procedure under anesthesia where the bladder is filled very fully with fluid. About one-third of patients feel better afterward.
Stress Management
Stress reduction, hypnotherapy, and acupuncture can have a beneficial impact for some people.
Illustrations courtesy of the International Urogynecological Association (IUGA) Patient Information Leaflets.